You’re Providing Care… But Billing Under the Wrong Provider
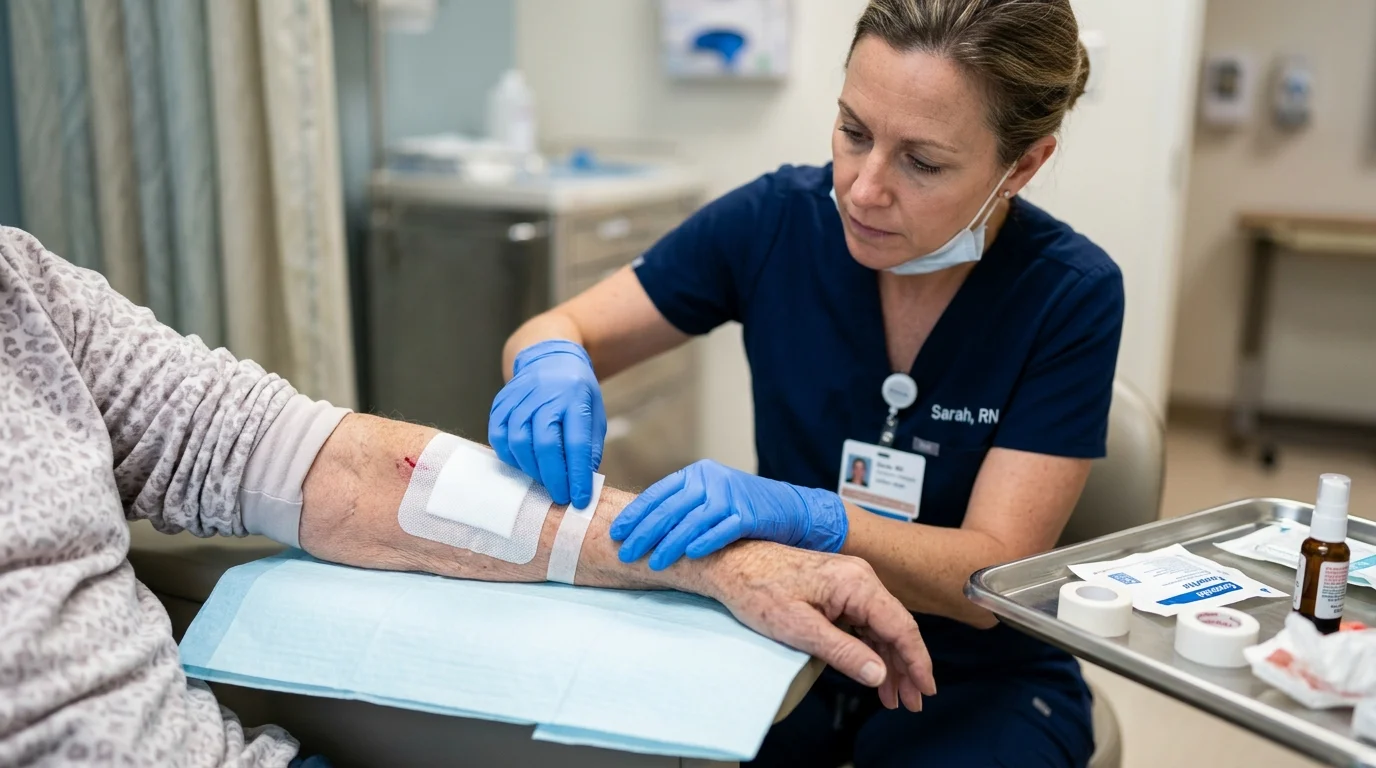
Your team is delivering care every day.
Nurse practitioners are seeing patients.
Physician assistants are managing follow-ups.
Care is being coordinated efficiently.
However, billing becomes confusing.
Behind the scenes:
- Claims get denied
- Provider names don’t match
- Supervision rules are unclear
- Compliance risks increase
So, you start wondering:
Are we billing incident-to correctly under Medicare?
For many practices—the answer is no.
What Is Incident-To Billing in Medicare?
Incident-to billing allows services performed by:
- Nurse Practitioners (NPs)
- Physician Assistants (PAs)
- Clinical staff
To be billed under a supervising physician’s NPI.
As a result:
- Reimbursement is typically higher
- The service is treated as physician-level billing
However, strict rules apply.
Why Incident-To Billing Matters
Medicare incident-to billing directly impacts:
- Reimbursement rates
- Compliance risk
- Audit exposure
Therefore, understanding the rules is essential.
Even small mistakes can lead to:
- Claim denials
- Overpayment recoupments
- Legal issues
Key Medicare Incident-To Billing Requirements
To bill incident-to correctly, all conditions must be met.
1. Physician Must Initiate Care
The physician must:
- Perform the initial service
- Establish the treatment plan
After that, staff can provide follow-up care.
2. Direct Supervision Is Required
The supervising physician must:
- Be physically present in the office
- Be immediately available
However, they do not need to be in the same room.
3. Established Patient Only
Incident-to billing applies only when:
- The patient is already established
- The condition is already diagnosed
New patients do not qualify.
4. Same Office Setting
Services must be provided:
- In a physician’s office
- Not in a hospital or facility setting
5. Following the Plan of Care
The service must:
- Follow the physician’s established plan
- Not introduce new problems
Otherwise, it cannot be billed incident-to.
Common Incident-To Billing Mistakes
Many practices make critical errors.
For example:
- Billing new patient visits as incident-to
- Physician not present during service
- Treating new conditions under incident-to
- Poor documentation of supervision
As a result, these mistakes often lead to audits and recoupments.
Incident-To vs Direct Billing (NP/PA)
Incident-To Billing
- Billed under physician NPI
- Higher reimbursement (~100%)
- Strict requirements
Direct Billing (NP/PA)
- Billed under provider’s own NPI
- Lower reimbursement (~85%)
- Fewer restrictions
Choosing the correct method depends on compliance—not just revenue.
Documentation Requirements
To support incident-to billing, include:
- Physician’s initial visit documentation
- Established plan of care
- Proof of direct supervision
- Notes showing follow-up care
Without proper documentation, claims may not hold up in audits.
How Incident-To Billing Impacts Your Revenue Cycle
When done correctly:
- Reimbursement increases
- Claims get approved faster
- Revenue improves
However, when done incorrectly:
- Denials increase
- Recoupments occur
- Compliance risks rise
Accuracy protects both revenue and your practice.
Best Practices for Incident-To Billing
To stay compliant:
- Train staff on Medicare rules
- Verify supervision requirements daily
- Audit documentation regularly
- Use correct billing pathways
By doing this, you reduce risk and improve billing outcomes.
Final Thoughts: Compliance Comes Before Revenue
Incident-to billing offers financial benefits.
However, it comes with strict rules.
When you follow guidelines correctly, you can:
- Maximize reimbursement
- Stay compliant
- Reduce audit risk
- Strengthen your RCM
Need Help with Medicare Billing Compliance?
If your practice is unsure about incident-to billing:
👉 Get a compliance audit
👉 Ensure proper billing and documentation
Let’s protect your revenue and reduce risk.