You’re Seeing Complex Patients… But Are You Billing at the Right Level?
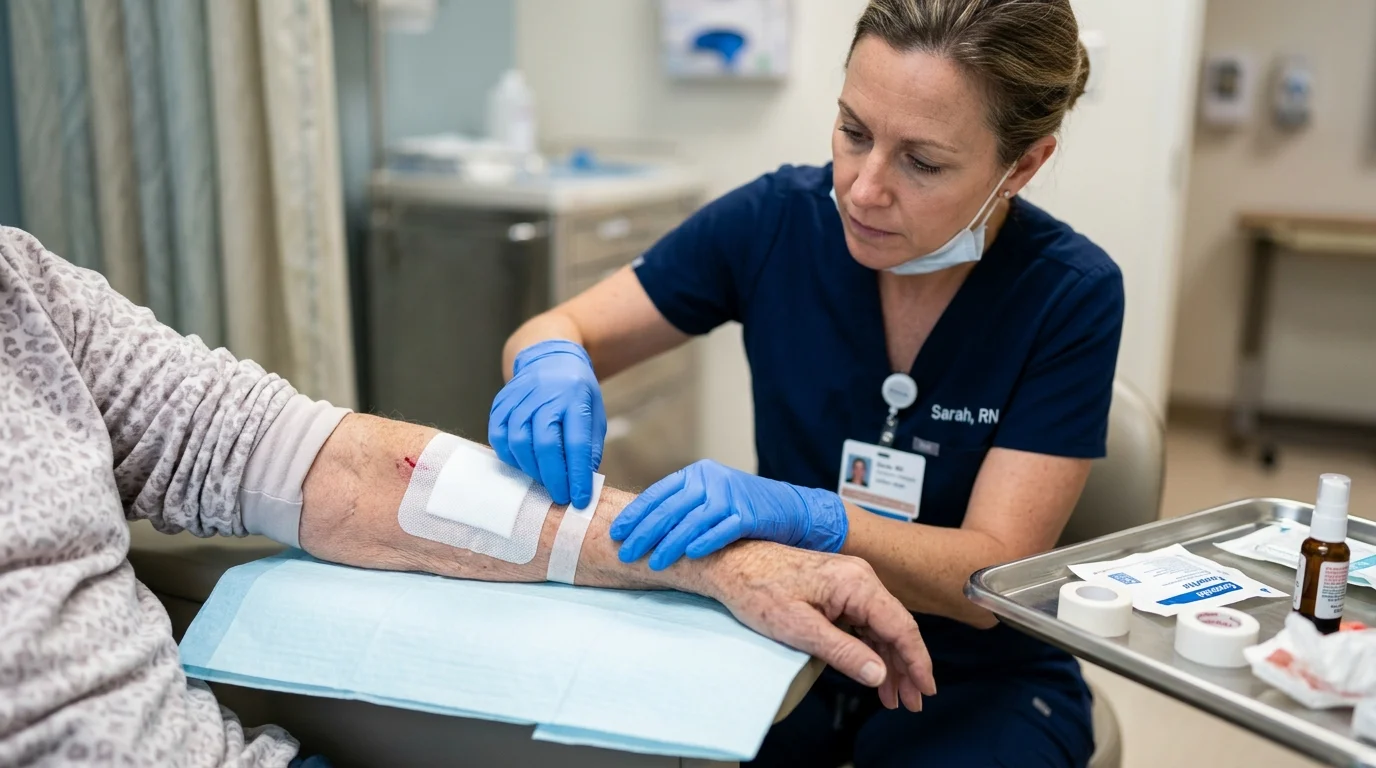
Your practice handles more than routine visits.
Patients present with multiple conditions.
Treatment decisions require deeper evaluation.
Risk levels increase.
However, billing often does not reflect this complexity.
Behind the scenes:
- Visits get undercoded
- Documentation lacks detail
- Reimbursement falls short
- Audit risks increase
As a result, you start asking:
👉 Should this visit be billed as CPT 99214?
What Is CPT 99214?
CPT 99214 is used for:
👉 Established patient office visits involving moderate complexity medical decision-making (MDM).
In simple terms:
- It represents higher complexity than 99213
- It applies to patients requiring detailed evaluation and management
- It reflects moderate risk care decisions
👉 Therefore, it is critical for capturing appropriate reimbursement.
When Should You Use CPT 99214?
You should report CPT 99214 when:
- The patient is established
- The visit involves moderate MDM
- The provider manages multiple or complex conditions
For example:
- Worsening chronic conditions
- Medication adjustments with risk
- Multiple diagnoses requiring coordination
👉 As a result, this code reflects more advanced clinical judgment.
Understanding Moderate Medical Decision-Making (MDM)
CPT 99214 is driven by MDM.
It includes three key elements:
✔ 1. Problems Addressed
- Multiple conditions
- Chronic illnesses with exacerbation
✔ 2. Data Reviewed
- Lab tests
- Imaging
- External records
✔ 3. Risk Level
- Prescription drug management
- Moderate risk of complications
👉 Therefore, documentation must clearly support all these elements.
Documentation Requirements for CPT 99214
To support this code, you must document:
- Detailed assessment of conditions
- Evidence of moderate MDM
- Data reviewed or ordered
- Risk factors and treatment decisions
👉 Without proper documentation, claims may be downcoded or denied.
CPT 99214 vs CPT 99213: Key Differences
Understanding this distinction is critical.
| Feature | CPT 99213 | CPT 99214 |
|---|---|---|
| Complexity | Low | Moderate |
| Conditions | Stable | Complex or worsening |
| Risk | Low | Moderate |
| Reimbursement | Lower | Higher |
👉 Therefore, selecting the correct level directly impacts revenue.
CPT 99214 Reimbursement Overview
Reimbursement depends on:
- Payer contracts
- Geographic region
- Facility vs office setting
However:
- CPT 99214 pays significantly more than 99213
- It is closely monitored for compliance
👉 Therefore, accuracy is essential.
Common Billing Mistakes with CPT 99214
Many practices struggle with this code.
✔ 1. Undercoding Moderate Visits
Providers often select 99213 instead.
👉 As a result, revenue is lost.
✔ 2. Overcoding Without Documentation
If documentation does not support MDM:
- Claims may be denied
- Audits may occur
✔ 3. Ignoring MDM Criteria
MDM determines the level.
👉 Therefore, guessing leads to errors.
✔ 4. Poor Documentation Structure
Incomplete notes create:
- Compliance risks
- Downcoding
How CPT 99214 Impacts Your Revenue Cycle
Correct usage leads to:
- Higher reimbursement
- Accurate coding
- Reduced denials
- Strong compliance
However, incorrect usage results in:
- Revenue loss
- Audit exposure
- Increased rework
👉 Ultimately, precision protects both revenue and compliance.
Best Practices for Accurate Billing
To optimize CPT 99214 usage:
- Document MDM clearly
- Capture all conditions addressed
- Record data reviewed
- Justify risk level
👉 Consistency ensures accurate reimbursement.
Final Thoughts: Complexity Must Be Reflected in Your Coding
CPT 99214 is not just a higher-level code.
It reflects the complexity of care you provide.
When used correctly, it allows you to:
- Capture full reimbursement
- Reduce undercoding
- Maintain compliance
- Improve financial performance
👉 The goal is simple: match your coding to the complexity of care.
Need Help Optimizing Your E/M Coding Levels?
If your practice struggles with:
- Undercoding complex visits
- Documentation gaps
- E/M audit risks
- Inconsistent billing
👉 It may be time to improve your coding strategy.
Here’s how we can help:
- ✔ E/M coding audits
- ✔ Documentation training
- ✔ Compliance support
- ✔ Revenue optimization
👉 Get a coding audit and uncover missed revenue opportunities.
Let’s ensure your coding reflects the care you provide.