You’re Seeing Patients… But Where’s the Revenue?
Your schedule is full.
Patients are coming in every day.
Care is being delivered.
Your team is working hard.
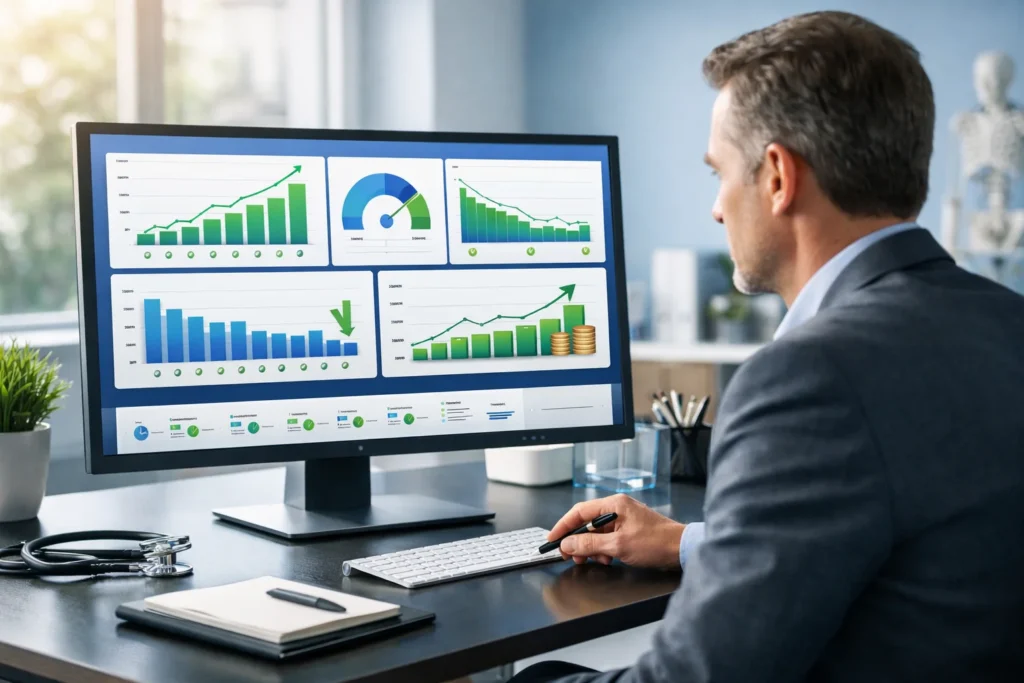
But when you look at your numbers—
- Payments are inconsistent
- AR is increasing
- Denials are piling up
- Collections feel lower than they should be
That’s when it hits you:
👉 “We’re doing the work… but we’re not getting paid properly.”
This is one of the most common challenges in healthcare—and it usually comes down to one thing:
👉 Inefficient Revenue Cycle Management (RCM)
What Does “Improving Collections” Actually Mean?
Improving collections isn’t just about chasing payments.
It means:
- Getting paid faster
- Getting paid accurately
- Reducing lost or delayed revenue
In a well-managed system, collections are predictable, consistent, and optimized.
That’s exactly what professional RCM services are designed to achieve.
What Are Professional RCM Services?
Professional RCM services manage the entire financial lifecycle of your practice.
This includes:
- Patient eligibility verification
- Medical coding
- Charge entry
- Claim submission
- Payment posting
- Denial management
- Patient collections
In short, they ensure that every step—from patient visit to final payment—is optimized.
Why Most Practices Struggle with Collections
Even high-performing practices lose revenue due to small inefficiencies.
1. Front-End Errors
Incorrect insurance verification or missing authorizations lead to denials later.
2. Poor Claim Accuracy
Incomplete or incorrect claims result in rejections and delays.
3. Weak Denial Management
Denied claims are often not followed up or reworked properly.
4. Lack of Visibility
Without proper reporting, practices don’t know where revenue is being lost.
5. Inefficient Patient Billing
Confusing statements and lack of follow-ups reduce patient collections.
How Professional RCM Services Improve Collections
Now let’s break down how RCM experts actually increase your revenue.
✔ Clean Claims Submission
RCM teams ensure claims are accurate before submission.
👉 Higher first-pass acceptance rate = faster payments.
✔ Reduced Denial Rates
Experts:
- Identify common denial patterns
- Fix root causes
- Resubmit claims quickly
👉 This directly recovers lost revenue.
✔ Faster Payment Cycles
With optimized workflows, claims move faster through the system.
👉 Lower AR days = better cash flow.
✔ Accurate Payment Posting
RCM teams ensure:
- Payments are recorded correctly
- Underpayments are identified
- Adjustments are applied properly
✔ Strong Patient Collections Process
Professional billing systems:
- Send clear patient statements
- Offer payment options
- Follow up consistently
👉 This improves patient payment rates.
✔ Real-Time Reporting & Insights
You get access to dashboards showing:
- AR days
- Collection rates
- Denial trends
- Revenue performance
👉 You can finally see what’s working—and what’s not.
The Role of RCM in USA Healthcare
RCM in USA is complex due to:
- Multiple insurance payers
- Changing regulations
- Strict compliance requirements
- Frequent coding updates
Without specialized expertise, practices often experience:
- Higher denial rates
- Delayed payments
- Revenue leakage
👉 That’s why professional RCM services are essential—not optional.
Key Metrics That Improve with Professional RCM
When RCM is optimized, you’ll see improvements in:
- Days in Accounts Receivable (AR) ↓
- Denial Rate ↓
- First-Pass Claim Acceptance Rate ↑
- Net Collection Rate ↑
👉 These metrics directly impact your financial health.
Why Practices Choose a Medical Billing Company in USA
Many practices partner with a medical billing company in USA to improve collections.
Because they provide:
- Certified coding expertise
- Advanced billing systems
- Dedicated denial management
- Scalable operations
👉 The result: more revenue with less stress.
Common Mistakes That Hurt Collections
Avoid these common issues:
- Skipping insurance verification
- Submitting incomplete claims
- Ignoring denial trends
- Not tracking KPIs
- Weak patient follow-up systems
👉 These small gaps lead to major revenue losses over time.
Final Thoughts: Collections Improve When Systems Improve
Improving collections isn’t about working harder.
It’s about working smarter.
When your RCM system is optimized:
- Payments become faster
- Revenue becomes predictable
- Stress decreases
- Growth becomes possible
Ready to Improve Your Collections and Maximize Revenue?
If your practice is struggling with low collections, high denials, or delayed payments:
👉 Get a free RCM audit for your practice today.
👉 Connect with our experts to improve your collections and streamline your revenue cycle.
Let’s turn your billing process into a high-performing revenue system.